Carbohydrate is one of the 3 main macronutrients in food, and is the one that has the greatest effect on glycemic control.
Controlling the amount of carbohydrate can help to control blood glucose. There are different strategies that might be used to assist in controlling carbohydrate, from simple to complex. The strategy used is individualized.
1. Consistent Carbohydrate
This strategy involves having a consistent amount of carbohydrate every day for each of breakfast, lunch, supper and snacks. It might be recommended as an initial strategy in someone who is newly diagnosed, with the idea that a more flexible strategy will be used later.
For some people, eating a consistent amount of carbohydrate is not a hardship, because they are very regular with their habits. For other people, this guideline is very restrictive.
Pros
- It is quick to teach, and to learn
- For people who are very regular with their eating, it comes naturally to them
- For people who are just starting insulin, it makes adjusting insulin doses easier
Cons
- It does not allow for flexibility in varying the carb content of meals day-to-day
Commonly used teaching materials include the AHS handout, Healthy Eating for Diabetes and the Diabetes Canada poster "Beyond the Basics".
2. Carbohydrate Budgeting
Carbohydrate budgeting refers to a strategy whereby a person has a specified amount of carbohydrate to consume at meals and snacks. The budget is often given as a range; a pretty standard guideline would be:
| Each meal | Each snack consumed | |
| Smaller eaters | 30-60 g carb (2-4 choices) | 15-30 g carb (1-2 choices) |
| Larger eaters | 45-75 g carb (3-5 choices) | 15-30 g carb (1-2 choices) |
Carbohydrate foods are grouped into portions (referred to as choices) that provide 15 g available carb per serving. Available carb is the carbohydrate that is digested and appears as glucose in the blood. It includes both starch and sugar, but does not include fibre.
Examples of foods and portions that count as 15 g available carb include:
- 125 mL (1/2 c) of potato, corn, pasta or cold cereal
- 1 medium apple or orange, 1/2 large banana, 250 mL (1 c) blueberries or 125 mL (1/2 c) unsweetened juice
- 250 mL (1 c) milk or fortified soy milk
- 15 mL (1 T) honey, sugar or syrup
Commonly used teaching materials (see below for links)
- Diabetes: Healthy Meal Planning
- Beyond the Basics
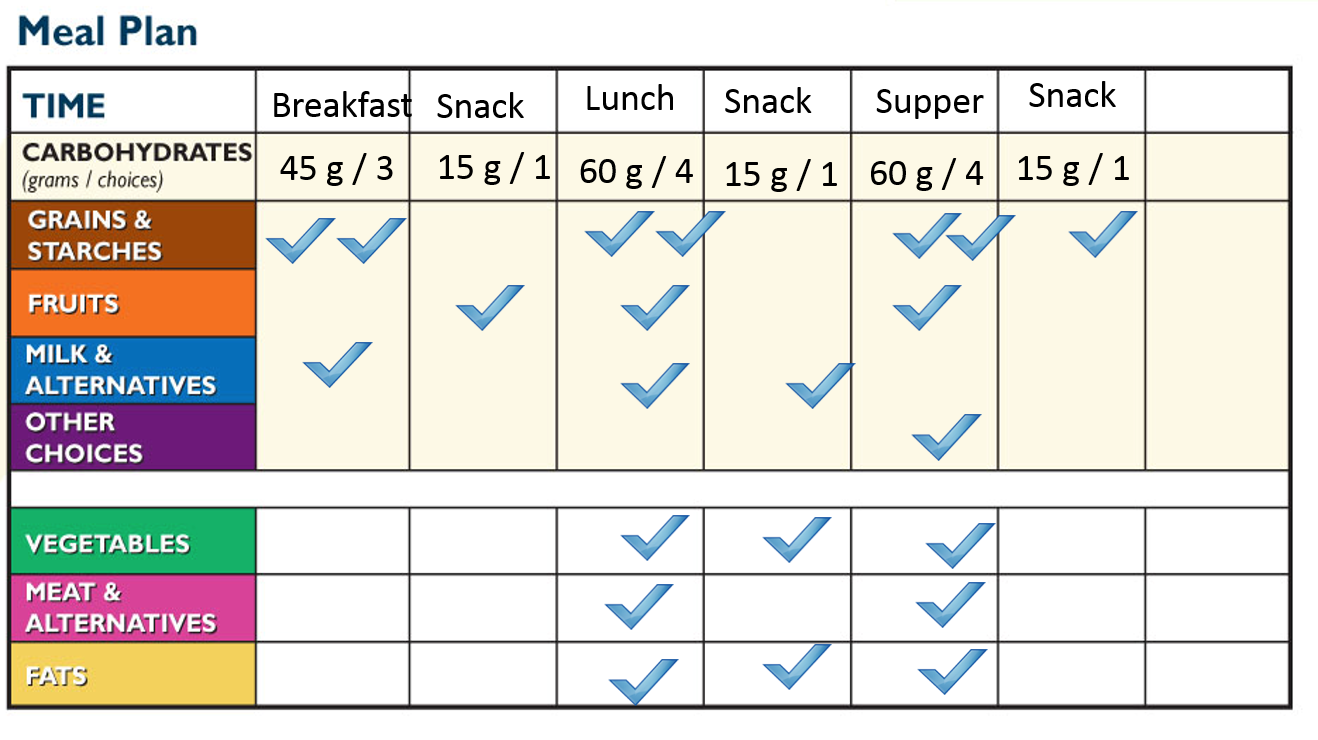
In the example meal plan shown above, the check marks are used to indicate an approximate number of choices to aim for at meals and snacks.
3. Simplified Carbohydrate Counting
A simplified form of carb counting has people adding up the number of carbohydrate choices as specifed above, and dosing bolus insulin for carb, based on that. As an example, a person might use the guideline of 1 unit insulin for 1 carb choice.
The strategy may work as a compromise for people who are not good at math and have trouble with more advanced forms of carb counting, but still allows for some variability in carb intake.
The concept may sometimes be used as a stepping stone to more advanced carb counting.
As an example only:
If the patient agrees to take 1 unit of rapid insulin for each carbohydrate choice, they might refer to one of the handouts noted. Given the following meal:
- 4 ounces steak (0 carb choices)
- 1 baked potato (estimated 1 cup = 2 carb choices)
- Salad (0 carb choices)
- 1 c milk (1 carb choice)
That adds up to 3 carb choices, so they would take 3 units of rapid insulin for the carbohydrate in the meal. Depending on the glucose reading prior to the meal, they may also add some correction insulin.
Commonly used teaching materials (see below for links)
- Diabetes: Healthy Meal Planning
- Beyond the Basics
- Carbohydrate in Foods
4. Advanced Carbohydrate Counting
This system is used to calculate the amount of bolus insulin to take for the grams of available carbohydrate being eaten. Typically, this is calculated only at meal times, but people on an insulin pump will bolus each time carbohydrate is consumed (unless the carb is to treat a low glucose). Intended carbohydrate consumption is added up, and the calculation to determine the amount of insulin to give is expressed as a Carbohydrate Ratio or Carb Ratio [formerly expressed as an Insulin:Carbohydrate Ratio (abbreviated as ICR)].
An example of a Carb Ratio is 12 (or ICR of 1:12). This means that each 12 g of available carbohydrate is estimated to need 1 unit of insulin.
An advanced modification that may be used by a few people, is to separately add the protein and fat being consumed, use another calculation to account for those, and add the units to the amount determined for the carb. This is not commonly used by patients, as it involves a lot of steps. Please refer to the Insulin for Protein and Fat page for more information.
Commonly used resources (see below for links)
To calculate the carbohydrate at a meal
- Nutrient analysis Apps
- Carb Counting Scale
- Restaurant websites
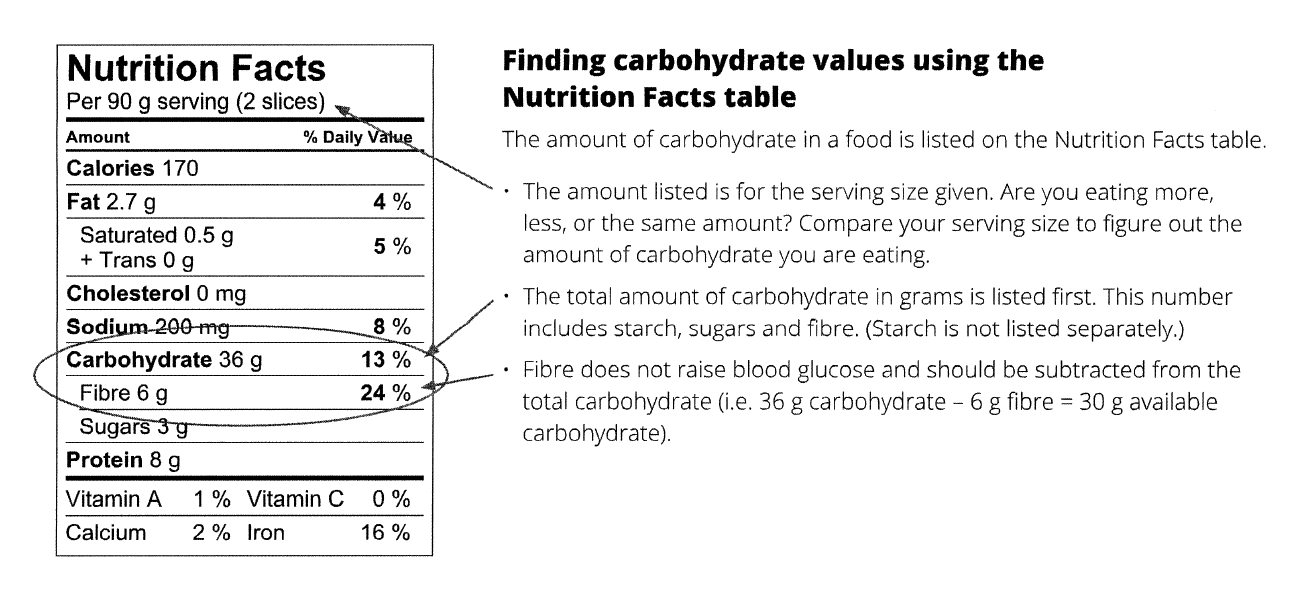
- Nutrition Facts label
To estimate an initial Carb Ratio, visit Insulin Formulas page.
For adjusting the Carb Ratio, visit Adjusting Insulin Page
Nutrition resources
A complete suite of AHS patient nutrition handouts are found on the NFS web page under "Diabetes".
Simplified resources include:
- "Carbohydrate in Foods" available on the AHS website: Nutrition Education Materials (Click on Diabetes)
- Basic Carbohydrate Counting (Diabetes Canada)
- Beyond the Basics from Diabetes Canada.
- Diabetes: Healthy Meal Planning is also found on the NFS web page under "Diabetes".
For advanced carb counting:
- Matching Insulin to Carbohydrates Handout
- Labels: Subtract grams of fibre from the grams of carbohydrate for the portion on the label.
- Nutrient Analysis Apps: Through smart phones' app stores or AppCrawlr
- Nutrient analysis websites or Nutrition Facts posted by restaurant franchises
- Carbohydrate Counting Scale (search on-line)